

NEWSLETTER
Enter your email here and receive updates
from TalesFromTheOrganTrade.com
Factoid Friday

This doctor built a custom dialysis machine from scratch in his garage to save a baby's life. At the time, there were simply no options for extremely small or premature babies.
Click here to read the article.

An old article, but this happened to make front page Reddit today.
Did you know there is only one country that has eliminated the shortage of organs—and it is the only country that has a legal payment system for organ donation?
Can you guess which country that is?
Click here to read the article.

Drinking too much cola (specifically cola, not soda in general) seems to increase the risk of kidney stones, renal failure and other conditions affecting the kidneys. In a study published in the journal Epidemiology, the team compared the dietary habits of 465 people with chronic kidney disease and 467 healthy people. After controlling for various factors, the team found that drinking two or more colas a day — whether artificially sweetened or regular — was linked to a twofold risk of chronic kidney disease.
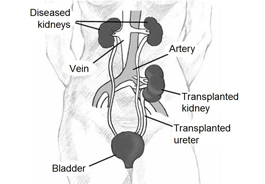
During a kidney transplant operation, your own failing kidneys are not actually removed. The new organ is placed in your pelvis rather than the usual kidney location in the back. The artery that carries blood to the kidney and the vein that removes blood from it are surgically connected to two blood vessels in the pelvis. The ureter, or tube that carries urine from the kidney to the bladder, is transplanted through an incision in the bladder. The entire operation takes between 2-4 hours.

Check out this archival footage of an artificial kidney demonstration (filmed in the 1960s):
Click here to watch.
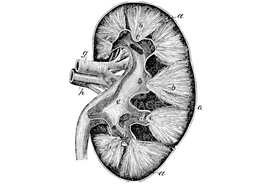
Etymology: Kidney(n.)
Early 14c., Middle English kidenei, kidenere (singular), kideneres, kideneren (plural); of unknown origin. Originally kidenere, perhaps a compound of Old English cwið "womb" + ey "egg" in reference to the shape of the organ. Figurative sense of "temperament" is from 1550s (of the same or a different kidney). Kidney bean is from the 1540s, so called for its shape.
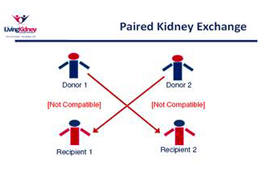
Kidney paired exchanges are becoming very common and an exciting option for kidney recipient and donor pairs who are not compatible with each other. Previously, people with kidney failure who had an incompatible donor were not able to benefit from the transplant being offered to them.
In Pair 1, Donor 1 is not compatible with Recipient 1. In Pair 2, Donor 2 is not compatible with Recipient 2. However, Donor 1 is compatible with Recipient 2 and Donor 2 is compatible with Recipient 1. If you, your donor and the other pair are willing to participate in this “exchange,” a comprehensive evaluation process begins. The medical team will complete final medical tests and schedule the transplant on a date that works with everyone. Both transplants usually occur at the same day. This example used 2 pairs, but in fact any number of pairs is possible.

On September 2, 1999, a human kidney was auctioned on Ebay. Bidding began at $25,000 and reached $5,750,100 before the company abruptly ended the auction.
Click here to read the article.

Check out this video from 1963! Here is the first patient to perform dialysis on himself (leading the way for home dialysis machines):
Watch it here!
A major breakthrough in the search for a cure for Type 1 Diabetes was just announced by Harvard University. Using stem cell technology, the Harvard team is now able to create functioning beta cells that produce insulin. Tests showed that the lab-made cells can control blood sugar levels in mice for several months. However, the beta cells cannot yet be injected into a person without facing immune assault.
As a side note, there is a company in San Diego called ViaCyte who appears to be a step ahead - ViaCyte is already performing cell replacement therapy trials on people.
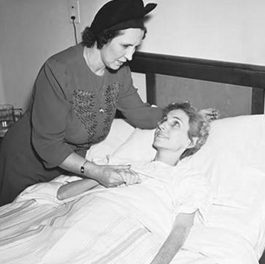
In this image from December 1940, "The Lady of the Golden Blood", Mrs. Rose McMullin comforts Mrs. Hazel Farmer at the American Hospital in Chicago before giving the ailing woman a half-pint of her blood. McMullin's blood was called "golden" because it was modified when she received a preparation of Staphylococcus aureus from her infected niece, and the child later made a complete recovery after her modified blood was transfused. In 1937, McMullin travelled to Pennsylvania to the home of another child dying of a similar infection, then to Chicago and Manhattan to help two more people. By 1940 she had reportedly given blood for over 300 transfusions.

As early as about 1920, archival photos show motorcycle riders wearing kidney belts. A kidney belt is a wide band around the lower torso that can protect a person's internal organs from strain or shock. In the 1920s, the roads were rutted and packed with dirt and gravel. In large towns, there were paving bricks. Motorcycles had no rear suspension, so you felt every little bump from the rear wheel through the frame and seat to your kidneys. Kidney belts are much less common since the arrival of rear shocks in the late 50’s, though they are still seen today on motocross riders and are also worn by some weightlifters, labourers and medical patients.
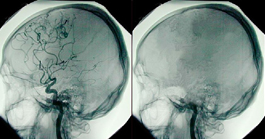
Brain death occurs when a person has an irreversible, catastrophic brain injury, which causes total cessation of all brain function. Brain death is synonymous with death; it is not a coma or persistent vegetative state. After a physician has declared a patient brain dead, organ donation is presented as an option to their family in order to give life to others.
The concept of brain death was proposed in the 1960s, but it's acceptance did not come easily. In 1968, Henry Beecher and the Harvard Ad-Hoc Brain Death Committee helped devise the criteria for brain death. Beecher wrote, "It is beyond question that a time comes when it is no longer appropriate to continue extraordinary means of support for the hopelessly unconscious patient. Secondly, a strong case can be made that society can ill afford to discard the tissues and organs of hopelessly unconscious patients so greatly needed for study and experimental trial to help those who can be salvaged. This can come about only with the prior agreement of society and finally approval in law."

The kidney is the primary organ for water homeostasis in the body. Water constantly escapes the body through sweat, urination, defecation or exhaled breath, and replacing these lost stores is essential. Every hour, a healthy kidney at rest can excrete 0.21 to 0.26 gallons of water and therefore a person can drink at a rate of 800 to 1,000 milliliters per hour without experiencing a net gain in water.
Individuals who chronically drink small amounts of liquid and cause themselves mild dehydration are at higher risk for urinary tract infections, kidney infections and kidney stones.
However, rehydration can be overdone. When a person drinks too much water in a short period of time, the kidneys cannot flush it out fast enough and the blood becomes waterlogged. Excess water leaves the blood and ultimately enters the cells, which swell to accommodate it. Inside the skull there is barely any room to expand and swell, and death may occur from brain swelling. We see this in long distance athletes attempting to rehydrate after an event, and in ecstasy users attempting to quench their thirst after a night of dancing and sweating.
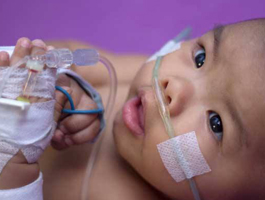
Until last year, babies with kidney failure were treated with machines built for adults. The number of infants around the world that suffer from kidney failure is very small, so it was risky for any company to invest in the technology.
Finally a fundraising program collected enough money to build a prototype and the CARPEDIEM (Cardio-Renal Paediatric Dialysis Emergency Machine) was born. The CARPEDIEM can be used on newborns and children up to 10kgs, can handle smaller volumes of fluid much more accurately, and allows the use of a much smaller catheter.
The first beneficiary, a girl with multiple organ failure, was treated in August last year. Nearly dead on arrival, she underwent 25 days of dialysis and went home in 50 days with her kidney function fully restored.

High blood pressure is a global epidemic and the leading cause of kidney disease, cardiovascular disease and stroke.
Just four hours of recreational exercise a week is proven to lower your risk of developing high blood pressure by twenty percent. But if you have a physically demanding job, you may not feel inclined to exercise on your own time for the health benefits. Interestingly, studies have found there is a difference between "occupational" and "recreational' exercise. Labour that involves the upper body - often the type that is performed on the job - can actually raise blood pressure, especially if strenuous. Physical activity on the job can be constant, repetitive, and there's usually external stress involved, which tends to lead to high blood pressure at the workplace.
It is important to exercise in a fun environment, such as playing a team sport, or on your own in a focused and low-stress environment. Try to incorporate lower body exercises like running and swimming, which are ideal for cardiovascular health and reducing blood pressure.

Here's a list of the top kidney-friendly foods (good for everyone, whether or not you have kidney disease):
1. Red bell peppers: Low in potassium while packing a generous serving of vitamins A, C, B6, folic acid and fibre.
2. Cabbage: High in vitamins K and C, B6, folic acid and fibre. Also low in potassium.
3. Cauliflower: Vitamin C, folate and fibre. Contains compounds that help your liver neutralize toxins.
4. Garlic: Reduces inflammation and lowers cholesterol.
5. Onion: Low in potassium, with anti-inflammatory properties.
6. Apples: High in fibre and anti-inflammatory properties.
7. Cranberries: Prevent urinary tract infections.
8. Blueberries: Contain plenty of vitamin C, fibre and manganese while also helping reduce inflammation.
9. Raspberries: Packed with fibre, vitamin C, folate, manganese and B vitamin.
10. Strawberries: Antioxidants, vitamin C, manganese and fibre.
11. Cherries: Cherries are filled with antioxidants and are shown to reduce inflammation when consumed daily.
12. Red grapes: Contain the flavonoid resveratrol which may help improve blood flow.
13. Egg whites: Provide high quality protein with essential amino acids, with less phosphorus than other proteins.
14. Fish: Another high quality protein with omega-3s.
15. Olive oil: Many beneficial components including inflammation-fighting oleic acid and antioxidants.

June 7, 1937: Hollywood is shocked to learn of the sudden death of actress Jean Harlow, who succumbs to acute kidney failure at the age of 26.
According to her obituary in the New York Times, the actress had suffered from poor health for a year, including “an acute case of sunburn,” a throat infection and influenza. She also contracted scarlet fever and meningitis as a teenager, which permanently weakened her health. After doctors diagnosed uremic poisoning the weekend before, according to the Times, “Miss Harlow soon responded favourably to treatment and was thought well on the road to recovery when she lapsed into a coma last night.”
Harlow is often considered the "original blond bombshell".
Four breakthroughs in the not-so-distant future:
1. Genomics: 10-15 years Finding the pathways by which structural abnormalities in the kidneys are formed, and then designing a molecule to block them.
2. Stem Cell Rejuvenation: Clinical trial in 5 years We can already form nephrons under the skin in mice. We just need to be able to do this within the structure of a kidney.
3. Implantable Artificial Kidney: 10 years Using nanotechnology and stem cell technology will produce an organ that can be hooked up to the vascular system and purify the blood.
4. Doubling the Life of the Transplanted Kidney: 5-10 years Through more precise suppression regimes and better understanding of biomarkers that first indicate rejection.
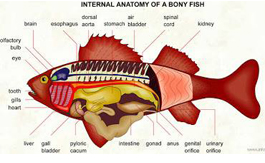
Ever wonder about the kidneys of other animals besides humans? All vertebrates have kidneys and the functional unit of the kidney in all species is the nephron.
Freshwater fish--like the zebrafish--have a long, tube-like kidney. The freshwater fish kidney functions mainly to create a dilute urine.
The frog kidney must be able to adapt to both freshwater and land conditions--thus the frog kidney must be able to create both a dilute and a concentrated urine, depending on the environment to which the frog is exposed.
Snakes live in a dry environment and therefore their kidneys must retain water. Snakes metabolize nitrogenous wastes into uric acid, which can be excreted in an insoluble form using very small amounts of water. The bird kidney also eliminates waste via uric acid.
Mouse kidneys are similar to human kidneys in that they use soluble urea, rather than insoluble uric acid, as the waste product.
The economic benefits of kidney transplants vs dialysis:
-The cost of in-centre hemodialysis is $83,000 per patient per year
-Home based dialysis such as peritoneal dialysis and home hemodialysis are less costly, from 30,000 to 58,000 per patient per year
-Overall, dialysis costs the healthcare system 2.5 billion per year
-The initial first year cost of a kidney transplant is $120,000 and follow up costs such as medication cost under $22,500 per year
-Over 5 years, each kidney transplant saves the health care system $200,000 compared to the most common form of dialysis
Kidney disease and aging:
Kidney disease can be diagnosed at any age, but the risk increases as we get older. After the age of 40, kidney filtration begins to fall approximately 1% per year. Other diseases that become more common with age - such as diabetes, high blood pressure and heart disease - are also a contributing factor.
It's estimated that one in five men and one in four women between 65-74, and half of people over 75, have some degree of CKD.

Can a woman who is on dialysis have a baby?
Some changes in your body, such as anemia and hormone changes, can make it difficult to become pregnant. A woman on dialysis is generally advised to avoid becoming pregnant, as risks to both the baby and mother are high. Close supervision and more frequent dialysis would be necessary to ensure a healthy baby.
A woman with mild kidney disease (stages 1-2) who is not on dialysis can usually become pregnant and have a healthy baby. A woman with a transplanted kidney can also have a healthy pregnancy, provided it has been at least one full year since the transplant.
Some things that can affect a healthy pregnancy include:
1. Your stage of kidney disease
2. Your general health
3. Your age
4. Having high blood pressure, diabetes, or heart disease
5. Having other serious health conditions
6. Protein in your urine

Kidney disease is often undetected in the general population, but children and teens are at a greater risk due to the ambiguity of the symptoms. Children might not be aware of changes to their body, and might not always let parents know.
If symptoms exist, they most commonly appear in the form of:
-Swelling of the hands and feet or puffiness around the eyes caused by excess fluid build-up
-Loss of appetite or increase in appetite
-Less frequent urination during the day
-Darker urine or extra foam in the urine that may indicate protein
-Headaches due to high blood pressure
-Nausea, vomiting, weakness, fatigue
-Difficulty concentrating or poor performance in school
Another indicator of potential kidney disease in children is family history of kidney disease. Genetic related disease is more common in children than adults.

Our kidneys filter harmful substances from our blood. One of these substances is alcohol.
Because of the kidneys' varied role, direct impairment of their function can result in a range of disorders, from mild fluid variations to acute kidney failure and even death. Our kidneys regulate levels of sodium, potassium, calcium and phosphate, which all play an important role in maintaining stable physical and chemical conditions around the cells; loss or retention of one of these substances due to alcohol consumption can affect the entire body. Scientists have observed alcohol-related changes to the structure and function of the kidneys, and impairment in their ability to regulate the volume and composition of fluid and electrolytes in the body. Alcohol can also compromise kidney function indirectly through liver disease or other conditions that force the kidneys to work even harder than usual.
Having more than three drinks in a day (or more than seven per week) for women, and more than four drinks in a day (or more than 14 per week) for men, is considered "heavy" drinking. The kidneys of heavy drinkers have to work harder. Drinking on a regular basis (or occasional binge drinking) has been found to double the risk for kidney disease. One drink could be a 12-ounce bottle of beer, one 5-ounce glass of wine, or one shot (1.5 ounces) of hard liquor.

The World Cup is here! Today, we take a look at three professional soccer players who developed kidney disease.
Clyde Simms: A former D.C. United midfielder, the 31-year-old was forced to retire this past February due to kidney disease. He is quoted saying "I made sure for as long as I could I would still fight for my dream, my passion. I was very lucky to have had such a great run, but now it's time for another battle." A young, healthy and active person, he wants to bring awareness to the fact that kidney disease can happen to anyone.
Ivan Klasnic: This former Werder Bremen and Bolton Wanderers striker was diagnosed with kidney disease in 2007. He quickly received a kidney from his mother, but it was soon rejected. A second transplant from his father was a success. He became the first player to ever return to a major tournament after undergoing a kidney transplant. Ivan blames the widespread abuse of painkillers, and the FIFA doctors who prescribe them. A recent study found that 39% of players take a painkiller before every game.
Hendrix 'Nguli' Banda (pictured): Hendrix passed away just last week from kidney failure. A former midfielder for the Malawi national football team, The Flames, he continued to coach upcoming talent even after his retirement from soccer.

About one in 750 people are born without one of their kidneys, according to the National Kidney Foundation. In the past, doctors believed it was best to restrict athletics to protect the remaining organ from acute kidney injury. However, recent studies have shown that injuries to the kidneys represent only a small percentage of the thousands of sports injuries reported every year. The risk of experiencing sports-related trauma pales in comparison to the risks to the kidneys and other organs posed by obesity, diabetes and other chronic diseases linked to inactivity.
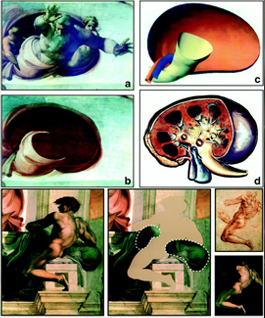
Sixteenth century artist Michelangelo had a lifelong interest in anatomy. Some speculate that his paintings on the Sistine Ceiling incorporated his familiarity with the structure and function of various organs. When the figures are removed, these images reveal what appear to be kidney shapes. Interestingly, there is evidence from his correspondence that Michelangelo may have suffered from kidney disease. This may account for his interest in anatomy and kidney function.
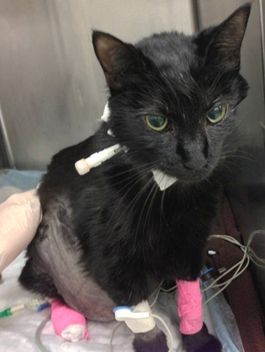
Dialysis can be used to treat acute or chronic kidney failure in pets. In some cases, particularly cats with chronic kidney disease, kidney transplantation may be available and would usually be preferred over dialysis. During the treatment, the animal sits in a quiet room on a cushioned table. Most animals take well to treatment and don’t seem to have the same degree of tiredness after dialysis that many people experience.

Dr. Irvine H. Page, shown on the October 31, 1955 cover of Time Magazine, played an essential role in the field of hypertension for almost 60 years. He discovered the link between heart disease and hypertension in 1948.
THE NEW YORK TIMES, New York, June 20, 1950
This 52 page newspaper has a small, somewhat discrete single column headline on page 30: "KIDNEY TRANSPLANT REPORTED SUCCESS".
Although the donated kidney was soon rejected because no immunosuppressive therapy was available at the time – the development of effective anti-rejection drugs was years away – Tucker's remaining diseased kidney began working again and she lived another 5 years before dying of an unrelated illness. The first truly successful kidney transplant occurred in 1954.
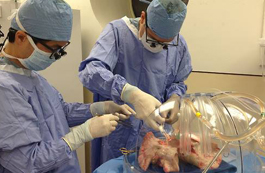
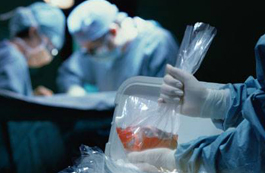
Transplant surgeons at the University of Pennsylvania performed the first ex vivo lung perfusion transplantation in 2012. The new technique repairs donor lungs that are damaged and unusable, allowing for successful transplantation of the reconditioned lungs. In this photo, Penn surgeons work on donor lungs in a sterile plastic chamber before transplantation into a patient.
Early transplant history: Russian surgeon Yu Yu Voronoy performed six human kidney allografts between 1933 and 1949 - in a bizarre twist, the attempted kidney transplants went into the thigh of the patient. The first 'successful' human-human kidney transplant lasted a mere 48 hours. The recipient was a 26-year-old woman who was admitted in a coma after swallowing mercury chloride in an attempted suicide. Voronoy retrieved the kidney from a 60-year-old man who had died from a fracture at the base of the skull.

Teddy Roosevelt's diary entry from the day his wife Alice died of kidney failure. Alice died two days after their daughter was born from undiagnosed kidney disease (in those days called Bright's disease), which had been masked by the pregnancy.
Yes, a dark thought for a Friday afternoon, but medicine has come a long way since 1884.
This March is Kidney Month -- we urge everyone to please take a moment to consider signing your donor card. You could save a life.

The kidney is the most common organ donated by living donors, though sometimes a living donor can donate part of their liver and in very rare cases part of their lung. The solid organs which can be donated by deceased donors are the heart, the liver, the pancreas, kidneys, the lungs and intestines. Check out this interactive map and graph for organ donation rates by country. Adding together the DBD (brain death donors) and DCD (cardio-circulatory death) rates yields a country's total deceased organ donation rate. Canada's rate was 14.7 PMP in 2012. We have a long way to go! Have you registered? http://public.tableausoftware.com/

Hippocrates (400 B.C.) described bubbles on the surface of the urine as indicating kidney disease and a long illness. Physicians inspected patient urine religiously for many centuries, carrying on with very little scientific evidence until the late 1700s. In 1655, Dr. Thomas Brian challenged the practice in his tract ‘The Pisse Prophet’. It was Richard Bright who conclusively demonstrated the association between proteinuria, dropsy and fatal kidney disease in 1827, and in doing so laid the ground for the specialty of nephrology.
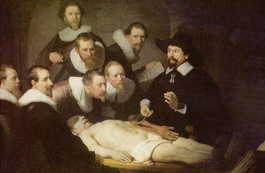
Nephrology (NEPHRO+OLOGY): a branch of medicine concerned with kidney function and diseases.
NEPHRO-: before vowels, nephr-, word-forming element meaning "kidney, kidneys," from nephro-, comb. form of Greek nephros "kidney".
-OLOGY: word-forming element indicating "branch of knowledge, science," now the usual form of -logy.
First known use of "Nephrology": circa 1842.
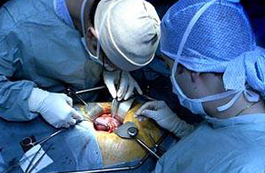
The success rate following kidney transplantation depends upon the closeness of the tissue match between donor and recipient. A kidney from a brother or sister with a “complete” match has a 95% chance of working at the end of one year. A kidney from a parent, child, or “half-matched” sibling has an 85% chance of working for at least one year. Finally, a cadaver donor kidney has an 80% change of working at least one year. All of these statistics assume this is your first transplant, and that you will be taking the anti-rejection drugs. For repeat transplants, the success rate becomes 10%-15% less.
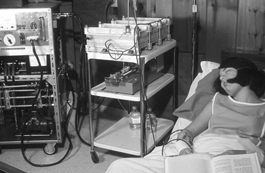
The first home hemodialysis patient in Seattle, WA. The Kiil dialyzer pictured here was used for overnight, unattended hemodialysis, which was developed in Seattle by Dr. Belding Scribner.
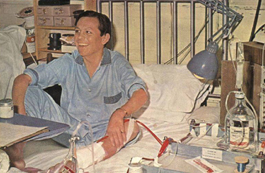
Perhaps the biggest problem in the early days of dialysis was an ethical one. Given the limited availability of facilities, how were the few patients who could receive treatment to be chosen from the many who needed it to stay alive? For several years, a committee composed of a minister, housewife, lawyer, banker, state government official, labour leader and surgeon were given the task of deciding which applicants would be admitted to the kidney centre. The committee came to be known as the "Life or Death Committee." They dissolved in 1967 (their function was no longer necessary as home dialysis became more common).
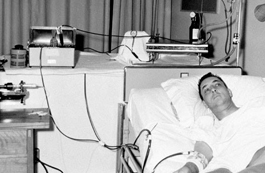
In 1960, kidney failure was a death sentence. Dialysis was mainly experimental and only used for a few days at a time. Dr. Belding Scribner of the UW School of Medicine took something that was fatal and turned it into 90 percent survival - literally overnight. "I woke up in the middle of the night with the idea of how we could save these people" recalled Scribner. The invention involved inserting a Teflon tube into the patient's vein and keeping access open by hooking the tubes together to allow a high blood flow "shunt".
Did you know:
Nearly 98% of all kidney transplants, 90% of liver transplants and 85% of heart transplants are successful! -Kin Canada
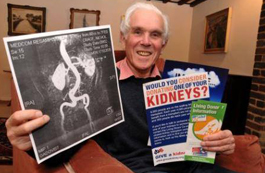
Myth: "I'm too old to be an organ donor."
Nicholas Crace, 83, became the oldest living organ donor when he donated one of his kidneys in 2012. Medical tests revealed that Mr. Crace's kidneys functioned as well as those of someone in their 40s.

In 1902, Dr. Alexis Carrel demonstrated the surgical joining of blood vessels to make organ transplantation feasible for the first time. The joining of blood vessels is one of many surgical techniques pioneered by the French doctor, who was awarded the Nobel Prize for Medicine in 1912.
6 in 10 Americans will develop kidney disease in their lifetime. Government estimates show 18 people die each day waiting for a transplant and every 10 minutes someone is added to the transplant list. Yearly costs for treating a patient on dialysis are nearly triple the costs for treating a transplant patient.
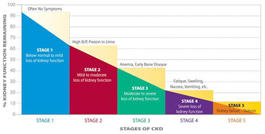
The five stages of kidney disease:
STAGE 1: Normal kidney function but urine findings, structural abnormalities or genetic traits point to kidney disease
STAGE 2: Mildly reduced kidney function and other findings (as for stage 1) point to kidney disease
STAGE 3: Moderately reduced kidney function
STAGE 4: Severely reduced kidney function
STAGE 5: Very severe, or end stage kidney failure
Most patients who are newly diagnosed with poor kidney function have a longterm condition which changes slowly. Acute renal failure occurs when there is a decline in renal function over hours or days - sometimes due to injury, bladder obstruction or drug use.
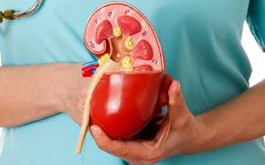
Did you know...
Kidneys maintain your body's metabolism (by regulating the levels of water and minerals).
Kidneys produce hormones, such as those that regulate blood pressure. If your kidneys shut down, you could die within days.
If diagnosed early, the progression of kidney disease can often be stopped.
Without medical intervention (dialysis or a kidney transplant) a person with kidney failure would die.
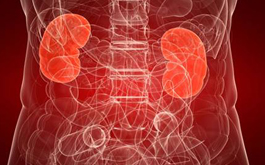
1 in 10 Canadians has kidney disease.
The number of Canadians being treated for kidney failure has tripled over the last 20 years.
The cost of treating kidney disease in Canada is over 2 billion dollars per year.
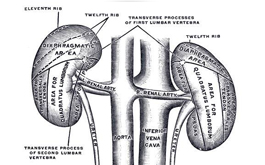
Human kidneys filter the body’s total blood supply about 12 times per hour.
A person may be born with one kidney, but it can adjust to filter as much as two kidneys would normally. If one kidney is missing from birth, the single kidney can grow to reach a size similar to the combined weight of two kidneys.
A very small number of people (approximately 0.07% of the population) are born with more than two kidneys. Two Latvian brothers found to have four kidneys each said it explained why they were able to drink their friends under the table.
Kidneys were once regarded as the seat of the conscience and reflection, and a number of verses in the Bible state that God searches out and inspects the kidneys of humans.

Chinese texts from 4th century BC contain the first account of organ transplantation, performed by surgeon Tsin Yue-Jen. According to the texts, the hearts of two soldiers were successfully exchanged - one with a strong spirit but a weak will and the other with the reverse - to cure the disequilibrium in their energies.

The basic concepts of nephrology and dialysis go back many centuries. In 100 AD, the citizens of Rome tried steaming in hot baths to sweat out toxins when they had a build-up of urea in their bodies.

Of the roughly 2 million Americans who die annually, less than 1% provide organs healthy enough for transplanting.

In the 16th century, the Italian plastic surgeon Gasparo Tagliacozzi performed successful skin autografts, but he failed consistently with allografts (skin from a different donor). Gasparo was the first to observe the immune response which his successors would come to recognize as transplant rejection.

Some famous people afflicted by kidney disease:
WOLFGANG AMADEUS MOZART, composer, died 1791 from likely kidney failure
EMILY DICKINSON, poet, died 1886 of Bright's disease
SARAH BERNHARDT, actress, died 1923 of kidney failure
JULIA CHILD, chef, died 2004 of kidney failure
NORMAN MAILER, author, died 2007 of acute kidney failure
MANUTE BOL, basketball player/activist, died 2010 of acute kidney failure
OSCAR PETERSON, jazz musician, died 2007 of kidney failure
BOBBY FISCHER, chess master, died 2008 of kidney failure
BARRY WHITE, singer, died 2003 of kidney failure
ART BUCHWALD, columnist and writer, died 2007 of kidney failure and diabetes

The world record for most people to sign up as organ donors in eight hours is 4,135! This was achieved by Dharmsinh Desai University in Nadiad, Gujarat, India, on January 1, 2013. The most people to sign up as organ donors in a single hour is 1,981, a record achieved by Antalya Provincial Directorate of Health in Antalya, Turkey, on March 1, 2013.
One organ donor can save up to EIGHT lives and enhance many more through tissue donation.
The current record for longest time spent on dialysis belongs to Brian Tocher, who has received haemodialysis for 33 years and continues 3 times a week. He began haemodialysis on June 13, 1966 and had two kidney transplants during this time which were unsuccessful.

Federal law bans the buying and selling of organs for transplantation; however it has not exclusively banned the use of organs for research, education and commercial endeavors. Advancements in biotechnology have generated new uses for human tissues. Cells and by-products have commercial value because human-made organisms may be patented, according to a 1980 ruling by the U.S. Supreme Court. The growth of the biotechnology industry and genetic research (not to mention the sale of hair, sperm and blood) has created a market for human parts despite the notion that "human body parts should not be viewed as commodities."
Image: Insulin crystals

Wait times for organs and tissues across Canada vary so much that some provinces have lists two to three times longer than in other regions (Albertans wait an average of three years vs. the eight year average in Ontario). This is because Canada does not have an integrated national registry - matching donors is done regionally and organs are seldom sent out of province. It is unlikely that this scenario will improve given the geography and the logistics of allocating organs in a country as large as Canada - especially because there is such a short window of opportunity for transplanting a cadaver organ.
table source: www.organsandtissues.ca
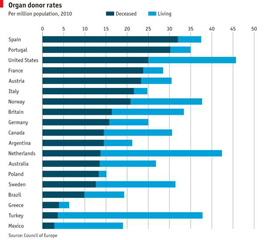
Organ donation rates by country.
The "Organización Nacional de Trasplantes" of Spain has an "opt-out" system for organ donation, and the highest number of deceased donors in the world. Experts question whether the "Spanish Model" would produce similar results if applied in other countries or if culture might be a better indicator of success (Greece also has an opt-out system and sits near the bottom of the list).
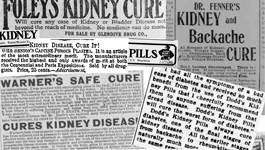
"KIDNEY DISEASE, CURE IT!" In the late 1800s, if a person were taken sick with kidney disease, his physician would consider their responsibilities at an end, for medical authorities admitted that the disease was incurable. However, this did not stop newspapers from advertising an array of "scientifically proven" miracle pills claiming to cure the disease.

Pressure Cooker Artificial Kidney - Inouye & Engleberg, 1952: A simplified artificial dialyzer and ultrafilter (previous models were bulky and weighed over 100lbs). Dr. Inouye took the original concept and miniaturized it by wrapping cellulose acetate tubing around a beaker and separating the layers with fiberglass screening. This coil was enclosed in a Presto Pressure Cooker to control the temperature. With the use of a vacuum he was able to draw excess water from the patient's blood. The device was used clinically and when it was used in a closed circuit, one could determine the exact amount of fluid removed.

The world’s first successful single-lung transplant was performed in Toronto in 1983, followed by the first double-lung transplant in 1986. Both transplants were performed by Dr. Joel Cooper of The University of Toronto. Canada is highly regarded for lung transplantation and the country’s lung transplantation rate is 5.3 per million population (PMP), compared to 4.7 PMP in the United States and 2.9 PMP in France.
Photo: Tom Hall (centre), world’s first single-lung recipient; Monica Assenheimer (left), second single-lung recipient; Ann Harrison (right), world’s first double-lung recipient
In 1983, Virginia physician H. Barry Jacobs proposed an International Kidney Exchange program. Jacobs wrote letters to 7500 hospitals outlining his plan to purchase kidneys for people on transplant lists, arguing that a voluntary donor system is to blame for the severe shortage in organ donors. His plan was met by widespread outrage. The National Kidney Foundation declared it "immoral and unethical". There were some parties however who supported the idea, such as Fortune magazine: "that's what markets are for - to give people, desperate or otherwise, a chance to optimize their own situations. Most people don't need two kidneys but do need to pay the rent occasionally."
The New York Times, November 1903:
"$5,000 will be paid for right ear, 2 1/2 inches long, 1 1/4 inches wide, with perfect curves and full lobe; the ear may be from male or female, and must be from a person in perfect health; offers by mail considered."
The very next day, German's Ear to be Bought" appeared in The New York Times.
"Skin Grafting" The Washington Post, Mar 25 1903

In 1891 a nurse at a San Francisco hospital, recently widowed, was compensated $100 when she allowed surgeons to scrape off 45 square inches of skin to treat a badly burned railway clerk. By 1903, skin had emerged as an "article of commerce" in several US cities including NY and Philadelphia. One reporter stated, "there is no reason why healthy men and women should not sell the article" after learning of a case in which a surgeon paid $5 for skin to help a badly burned child.

When South African surgeon Christiaan Barnard transplanted the heart of a "Cape coloured man" into the body of a white dentist in 1968, many noted the irony that the "coloured man's heart" could now enter hundreds of places still restricted to whites only. The operation aroused racial controversy in the U.S. as well. There was concern that doctors - already feared for using black patients as experimental subjects - would hasten the deaths of black patients so that their organs could be harvested for wealthy, white recipients.

In the early 20th century, occasional rumours circulated about the selling of solid tissue – skin, ears, and especially male generative glands. The first expressions of concern about traffic in organs arose in the 1920s. Authors and filmmakers began to incorporate the sale of body parts into fiction and film. In 1984, US Congress passed the 'National Organ Transplant Act' which outlawed the buying and selling of human organs.

2005: Johns Hopkins Medical Center pioneers the "domino chain" method of organ donation. The procedure takes a group of incompatible donor-recipient pairs (recipients who visit a hospital with a willing donor who is not compatible by blood or tissue) and matches them with other pairs in a similar predicament. Last year, a record sixty-person domino chain was completed.

Mary Shelley's Frankenstein describes a morally and physically superior creature constructed with parts from graveyards; this creature turns to violence only when his fictional creator rejects him. This is the first positive and negative depiction – in literature and "media" – of the use of organs and parts from dead people.
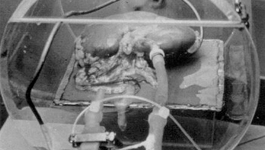
In the 1960's, Dr. Folkert O. Belzer developed a perfusion preservation machine that allowed organs to be kept viable longer. In 1987 he helped develop the "UW solution," a fluid that could keep donated organs viable from 18 to 30 hours. The extra time allowed for better matching of organs and recipients - thus decreasing the chance of rejection.

Dr. Karl Landsteiner is the first to classify human blood into the groups A, B, O, and AB, thus enabling physicians to transfuse blood - and later to transplant organs - without endangering a patient′s life. Individuals with the blood group AB are referred to as 'universal recipients' and those with blood group O are known as 'universal donors'.
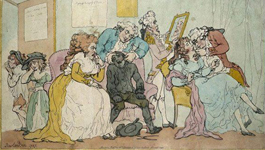
In the 18th century, before dentures, it was common for affluent Europeans to replace lost or rotten teeth with healthy teeth purchased from another person. The sellers were typically impoverished and desperate, and the practice faced criticism. Modern dentistry has eliminated the market for human teeth, but the selling of human body parts is a flourishing global industry. For some, moral condemnation is relative - especially when it's a matter of life or death.

Dr. Joseph E. Murray performed the first successful organ transplant in 1954, when he removed a healthy kidney from a 23-year-old man to save the man’s ailing identical twin.

The first practical dialysis machine was developed in 1943 by Dutch physician Dr. Willem Kolff.
www.apltd.ca










